Let me start with a confession: when was the last time you asked, “Is what my doctor prescribes actually the best for me?” I grew up in a house with more cakes than carrots, and conversations on heart health rarely made the dinner table. But everything changed after I watched a close family member fall to a sudden heart event—a tragedy that nudged me to look beneath glossy medical advice. In 2024, the world of medicine juggles vaccine updates and surging skepticism about drug reliance. We’re overdue for an honest chat about what’s really keeping us healthy—and what might be getting in the way.
When Numbers Shock: Heart Attacks, The Vaccine, and the Data We Ignore
Sometimes, the numbers you hear in the news don’t just surprise you—they force you to stop and rethink what you know about health, medicine, and the systems we trust. Imagine getting a call, as Dr. Malhotra did, from a journalist who says,
"We've got reports now of a 25% increase in heart attacks in hospitals in Scotland which are unexplained."(0.26-0.31). That’s not a small uptick. It’s a spike that makes you wonder: what’s really going on beneath the surface?
This sudden rise in heart attacks following the COVID-19 vaccine rollout in Scotland has left many experts and patients alike searching for answers. While correlation doesn’t always mean causation, the timing has led to tough questions about vaccine safety surveillance and the broader landscape of medical risk. COVID-19 vaccine effectiveness estimates are a key part of public health messaging, but so is transparency about possible side effects—even if they’re rare or still being investigated.
Research shows that the 2024–2025 COVID-19 vaccine demonstrates 33% effectiveness against COVID-19-associated emergency department or urgent care visits among adults aged 18 and older during the first 7–119 days after vaccination. That’s a significant number, but it also means that a majority of vaccinated adults may still experience breakthrough infections requiring urgent care within that window. This is why ongoing vaccine safety surveillance remains so crucial. It’s not just about promoting COVID-19 vaccine safety; it’s about ensuring that the data is clear, up-to-date, and openly discussed.
But the story doesn’t end with vaccines. When you zoom out, you see that prescribed medications as a whole carry their own risks. As Dr. Malhotra points out,
"A credible estimate suggests the third most common cause of death globally after heart disease and cancer is prescribed medications."(0.50-0.57). This is a startling fact that rarely makes headlines. It’s a reminder that while drugs can save lives, they can also cause harm—sometimes on a massive scale.
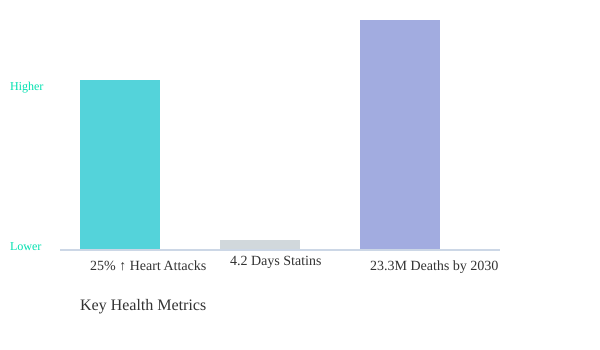
Take statins, for example. Over 200 million people worldwide take these medications to lower cholesterol and reduce the risk of heart disease. Yet, studies indicate that the average increase in life expectancy from statins is just 4.2 days over five years. That’s a modest gain, especially when weighed against potential side effects and the psychological impact of daily medication. Meanwhile, heart disease remains the world’s leading killer, with projections estimating 23.3 million annual deaths by 2030.
So, where does this leave you? It’s clear that both COVID-19 vaccine effectiveness and the safety of other widely prescribed drugs deserve ongoing scrutiny. The numbers are big, and the stakes are high. Personalized healthcare isn’t just about following guidelines—it’s about understanding the risk/benefit math for yourself and being willing to ask uncomfortable questions, even when the answers aren’t simple.
As you look at the data—whether it’s the 25% increase in heart attacks in Scotland, the modest benefits of statins for 200 million users, or the projected surge in heart disease deaths—one thing becomes obvious: the conversation about health must go deeper. It’s not enough to accept the surface-level story. You need to dig into the numbers, challenge assumptions, and demand transparency from the systems that shape your care.
Medicine’s Dirty Secret: Overprescription, Commercial Influence, and Trust Erosion
When you look beneath the surface of modern medicine, a troubling reality emerges: prescribed medications are now recognized as the third leading cause of death globally, right after heart disease and cancer (0.50–0.57). This is a “dirty secret” within healthcare, rarely discussed openly, but it’s crucial to understand how we got here—and what it means for your trust in the system.
Pharmaceutical Influence: Shaping Prescriptions and Perceptions
Pharmaceutical companies wield enormous influence over both prescription habits and the way health outcomes are perceived. As one expert put it,
“Medical knowledge is under commercial control—this is the root of the problem.”(0.41–0.44). This commercial control doesn’t just affect what drugs are prescribed; it also shapes the data doctors see, often exaggerating benefits and downplaying risks. Research shows that doctors may rely on incomplete or biased information, leading to overprescription and, ultimately, harm.
Drug Prescriptions: Life-Saving or Life-Threatening?
It’s true that many medications save lives. But the scale of harm is staggering. One credible estimate suggests that prescribed drugs are responsible for more deaths than most people realize—making them the third most common cause of death worldwide (0.50–0.57). The system, as described by critics, can be “psychopathic when it comes to making money, and there is so much harm that comes from drug prescriptions” (0.44–0.48).
| Global Cause of Death | Estimated Rank | Notes |
|---|---|---|
| Heart Disease | 1st | Leading global cause |
| Cancer | 2nd | Second leading cause |
| Prescribed Medications | 3rd | Linked to overprescription and commercial influence |
Trust Erosion: When Transparency Lags Behind
Public trust in medicine is fragile. When transparency about drug safety lags behind emerging evidence—or appears to be shaped by commercial interests—patients are left questioning what (and who) to believe. This is especially relevant in the context of vaccine safety surveillance and vaccine safety monitoring, where real-time, unbiased data is essential for public confidence.
For example, the FDA and CDC have expanded public access to vaccine safety data in 2025, aiming to enhance transparency and rebuild trust. Vaccine safety passive surveillance systems, like VAERS, are now more accessible, but skepticism remains. Studies indicate that ongoing vaccine safety monitoring is vital, especially as new COVID-19 vaccine safety data for 2025 emerges and recommendations evolve.
First, Do No Harm: An Ethical Imperative Lost?
The phrase “First, Do No Harm” is more than a documentary title—it’s a foundational medical ethic. Yet, in a profit-driven system, this principle can be overshadowed by commercial priorities. Patients are often left navigating a confusing landscape of hype, science, and commercial interest, unsure where to place their trust.
- Doctors may not always have access to unbiased data.
- Patients struggle to interpret conflicting information.
- Commercial interests can undermine both safety and trust.
As you consider your own health decisions—whether about heart disease, statins, or the latest COVID-19 vaccine—remember that true vaccine safety surveillance and responsible prescribing require transparency, ethics, and a commitment to putting patients first.
Lifestyle over Lifelines: Statins, Sugar, and the Power of Choice
When you look beneath the surface of modern healthcare, you’ll find a striking reality: heart disease is projected to claim 23.3 million lives each year by 2030 (1.11–1.15). This staggering figure highlights the urgent need for broader prevention strategies that go beyond prescriptions and quick fixes. The facts about statins—one of the most widely used drugs for heart health—are eye-opening. Over 200 million people globally take statins, yet research shows the average increase in life expectancy is only 4.2 days over a five-year period (1.17–1.23). These statin facts challenge us to rethink what true prevention really means.
| Statistic | Value |
|---|---|
| Projected annual heart disease deaths by 2030 | 23.3 million |
| Global statin users | 200 million |
| Statin life expectancy gain (5 years) | 4.2 days |
It’s easy to focus on numbers—cholesterol, muscle mass, abdominal fat—and forget what’s happening inside your body. Many people obsess over appearance metrics, but these can distract from the real markers of health, like cardiovascular function and metabolic balance. Sometimes, you don’t realize your heart health is at risk until symptoms appear or a crisis strikes (1.26–1.30).
For many families, the struggle with chronic illness is deeply personal. Maybe you’ve seen relatives battle processed food addiction, especially sugar, and watched as these habits led to long-term health issues. These patterns often repeat across generations, shaping not just individual lives but the health of entire communities. If you recognize these cycles in your own life, you’re not alone.
That’s where Lifestyle medicine comes in—a powerful, yet often underutilized, approach to preventing and even reversing heart disease. Instead of relying solely on medications, lifestyle medicine emphasizes nutrition, regular exercise, stress management, and sleep. Studies indicate that lifestyle changes offer greater long-term benefits to heart health compared to most standard drug interventions. This isn’t just theory; it’s supported by decades of research and real-world results.
As one expert put it,
"We should shift our approach to health from a predominantly drug-based model...to one which is more based upon lifestyle."
(2.54–3.10)
Why does this shift matter? Because empowering you to prioritize true prevention means changing the focus from drugs to daily habits. When you understand that statins provide only modest improvements, it becomes clear that the real power lies in your everyday choices. Simple actions—like preparing meals from whole foods, moving your body, and managing stress—can have a profound impact on your long-term health.
It’s also important to recognize that heart health is often overlooked until it’s too late. Many people don’t seek help or make changes until they experience a major event, like a heart attack. By then, the options may be more limited. That’s why prevention through lifestyle medicine is so critical—it gives you the tools to protect your health before problems arise.
In the context of broader public health, these lessons resonate with current discussions about COVID-19 vaccine effectiveness, COVID-19 variants protection, and vaccine effectiveness by age. Just as with heart disease, prevention and proactive choices remain at the core of lasting health. The more you know about your options, the more empowered you become to make choices that support your well-being for years to come.
Doctors Under Pressure: The Human Cost of a Strained System
When you think about the people behind your healthcare, it’s easy to imagine doctors as resilient, almost superhuman. But beneath the surface, the reality is far more complex—especially in systems like the NHS, where the pressure is relentless. As Dr. Malhotra shares, “Within the NHS... we have the highest capita population per doctor in Europe... and the most number of doctors on night shift” (6.25-6.40). This means fewer doctors per patient and more night shifts than anywhere else in Europe, leading to significant burnout risk and, sometimes, heartbreaking consequences for both patients and their families.
If you’ve ever wondered how these pressures affect care, consider the sheer volume of patients a single cardiologist might see. Over a career, doctors like Dr. Malhotra have managed tens of thousands of cases (6.53-6.58). That kind of experience brings expertise, but it also brings exhaustion. The workload is so intense that even the most dedicated professionals can struggle to balance compassion with the need to keep moving, patient after patient.
For Dr. Malhotra, medicine is personal. He grew up in a medical family, and the loss of his older brother to heart disease left a deep mark. His brother, who had Down syndrome and a small hole in his heart, died suddenly at age 13 after a viral infection led to myocarditis—a rare but devastating complication (7.14-8.14). It’s a reminder that heart health isn’t just about numbers or statistics; it’s about real people, real families, and the unpredictable nature of disease.
The strain on the system doesn’t just impact chronic conditions like heart disease. Acute emergencies—whether it’s a heart attack or a severe infection—can expose the cracks in healthcare infrastructure. Dr. Malhotra’s mother, a GP who dedicated 25 years to the NHS, suffered for years with rheumatoid and osteoarthritis. When she developed sepsis, the system was simply too stretched to respond effectively. “It was heartbreaking to watch her suffer slowly over a number of years, but the way she was failed by the NHS specifically is that... the system was under so much strain” (12.32-12.39).
These stories aren’t just anecdotes; they reflect a broader pattern. Research shows that understaffed health systems compound risks for both chronic and acute care, making missed opportunities and delayed responses more likely. This is especially relevant as we look at the public’s trust in healthcare recommendations—like those from the CDC and ACIP on COVID-19 vaccine safety. When emergency department visits surge, or when new vaccines are rolled out, the ability of the system to respond quickly and safely is put to the test.
You might not always see the human cost of a strained system, but it’s there. Medical professionals are constantly asked to balance evidence-based care with empathy, even as their own resources are stretched thin. True compassion in medicine shines brightest when doctors have the time and space to offer personalized care—not just follow protocols. But as the system stands, that’s becoming harder to achieve.
The lesson here is clear: systemic reform isn’t just about numbers or efficiency. It’s about protecting the well-being of both patients and those who care for them. As public trust in COVID-19 vaccine safety and recommendations remains crucial, so too does the need to support the people who make healthcare possible—especially when every emergency department visit, every diagnosis, and every life saved depends on their resilience.
Who Gets Protected? Effectiveness, Age, and the Tough Questions We Shouldn’t Avoid
When you think about COVID-19 vaccine effectiveness, it’s easy to get lost in numbers and recommendations. But the reality is, who gets protected—and how well—depends on your age, your health, and the ever-changing landscape of viral variants. The CDC and ACIP recommendations for the 2024–2025 COVID-19 vaccine reflect this complexity, urging everyone aged 6 months and older to get the latest dose targeting Omicron JN.1 and its sublineages. But what does that mean for you, especially if you’re older or have underlying health conditions?
Vaccine Effectiveness by Age and Immune Status
Research shows that vaccine effectiveness is highest shortly after vaccination, but it’s not the same for everyone. For immunocompetent adults aged 65 and older, the 2024–2025 COVID-19 vaccine offers about 46% protection against hospitalization in the first 7–119 days after vaccination. If you have immunocompromising conditions, that number drops to 40%. For adults 18 and older, effectiveness against emergency room or urgent care visits is around 33% in the same window.
These numbers might seem modest, but they have real-world impact. During the 2023–24 respiratory season, COVID-19 vaccination averted approximately 68,000 hospitalizations. That’s not just a statistic—it’s thousands of families spared the anxiety and disruption of a loved one in the hospital.
Updated Vaccines for a Changing Virus
The virus keeps evolving, and so do the vaccines. The 2024–2025 COVID-19 vaccine is updated to match the circulating Omicron JN.1 variant and its relatives, aiming to maintain protection as the virus shifts. According to CDC and ACIP recommendations, this universal approach is meant to simplify decisions and maximize community protection. As the guidance states:
“CDC and ACIP recommend that all persons aged ≥6 months receive the 2024–2025 COVID-19 vaccine dose targeting Omicron JN.1 and derived sublineages.”
Still, the level of protection you get may depend on your age and immune status. Booster shots remain advised, especially for those at higher risk.
Safety Monitoring: Ongoing and Transparent
Vaccine safety is never a finished story. The FDA and CDC continue to monitor COVID-19 vaccine safety through both passive and active surveillance systems. In 2025, public access to VAERS (Vaccine Adverse Event Reporting System) data was expanded, increasing transparency and allowing you to see reported side effects in near real-time.
“The FDA monitors COVID-19 vaccine safety through both passive and active surveillance systems.”
Ongoing surveillance and public inquiry are vital. The safety profile of the 2024–2025 COVID-19 vaccine remains similar to earlier versions, but as with any medical intervention, vigilance is key.
Why Age and Health Still Matter
If you’re over 65 or have health conditions that compromise your immune system, you face a higher risk of severe COVID-19 outcomes. The vaccine offers significant, though not absolute, protection. It’s a layer of defense, not a guarantee. This is why CDC and ACIP recommendations emphasize boosters and updated doses for these groups.
It’s also a reminder that vaccine effectiveness by age and underlying health is just one part of the picture. As the transcript (9.11–10.55) highlights, heart health and chronic conditions play a huge role in outcomes—not just for COVID-19, but for overall well-being. Globally, heart disease is expected to claim 23.3 million lives annually by 2030, making preventive health measures, including vaccination, all the more urgent.
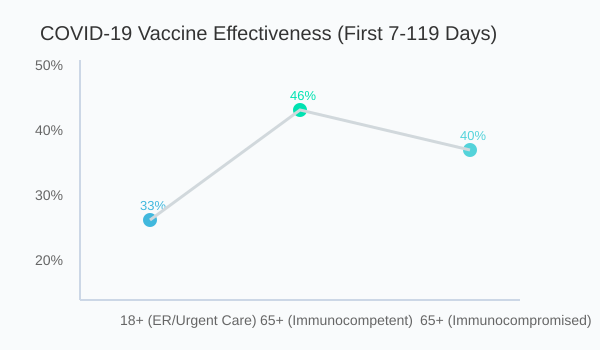
Chart: COVID-19 vaccine effectiveness against hospitalization and urgent care visits by age group and immune status, first 7–119 days after vaccination. Source: CDC, 2024–2025.
Wild Cards & Tangents: Analogies, Anecdotes, and What We Wish We’d Known
Imagine you’re driving a car. Now, picture if the manufacturer decided to dim your dashboard’s warning lights—just enough that you might miss a critical alert. That’s a bit like what happens when we rely only on optimistic vaccine safety data, without full transparency. In medicine, especially when it comes to COVID-19 vaccine safety, the stakes are much higher than a missed oil change. If we don’t see the whole picture, we risk missing early signs of trouble.
Dr. Malhotra’s story brings this home in a way that statistics never could. He grew up in a medical family (7.14-7.19), with both parents as doctors and an older brother, Steve, who had Down syndrome and a small hole in his heart (7.19-7.26). When Dr. Malhotra was just 11, his brother caught what seemed like a simple stomach bug. Within six days, Steve became breathless, deteriorated rapidly, and died after a cardiac arrest (7.29-7.47). The postmortem revealed a massively enlarged heart—viral myocarditis, a rare but devastating complication. As Dr. Malhotra explained, “
Instead of dealing with a cold on its own, the body then attacks the heart...and in a third of those patients, they deteriorate and die.” (8.05-8.11)
This kind of personal loss leaves a mark. It shapes how you view medical risk, and what you wish you’d known sooner. For Dr. Malhotra, it became a motivation to help others manage unseen dangers—those that don’t show up until it’s too late. It’s a reminder that the most important health risks are often invisible, like the foundations of a house. You rarely think about your heart or brain, because you can’t see them. But when something goes wrong, the consequences are profound (8.36-9.01).
Now, let’s take another analogy. What if prescription guidelines were written by chefs? Would you be told to have statins with every meal, or would you learn to cook for your health? Sometimes, medical advice can feel like a recipe handed down without explanation—do this, take that, trust us. But real trust, especially in COVID-19 vaccine public trust, isn’t inherited. It’s earned, through honest conversations, open data, and a willingness to answer tough questions.
That’s why access to vaccine safety data and systems like VAERS data access matter so much. Research shows that credibility in medicine—and vaccines specifically—depends on transparency and the willingness to examine dark corners, not just bright spots. If you only hear about the benefits, but never the risks or uncertainties, it’s like driving with those dimmed warning lights. You might get where you’re going, but you’re taking a chance you don’t need to.
Analogies and tangents aren’t just storytelling tricks. They help uncover the gaps in public understanding and highlight where the system needs to be more open. When you hear a personal narrative, like Dr. Malhotra’s, it’s easier to see both the benefits and the hidden costs of current medical practice. It’s a call for more transparent discussion—a reminder that the future of vaccine and drug credibility will depend on continual honesty, open data, and making room for questions that don’t always have easy answers.
Conclusion: If True Health Starts at Home, Where Does the Medical System Fit?
When you think about your health, it’s easy to picture the doctor’s office, the hospital, or the latest prescription. But real health—lasting, resilient health—often starts at home. It’s shaped by your daily choices, your habits, and your willingness to ask questions. In 2024, as we navigate new challenges in public health, vaccine safety surveillance, and heart health, it’s time to rethink where the medical system fits in your journey.
Reclaiming Responsibility: The Patient’s Role
You have more power than you might think. Whether it’s about the latest COVID-19 vaccine effectiveness data or the risks and benefits of heart medications, your voice matters. Patients today can and should demand more transparency and less dogma. If something doesn’t make sense, ask for clarification. If a recommendation feels rushed or one-sided, seek a second opinion. This isn’t about being combative; it’s about being an informed partner in your own care.
Consider the story at 12.57-13.07 in the transcript, where a patient’s mother was admitted to the hospital with a severe infection. Her frailty and weakened immune system, likely worsened by years of arthritis, made her more vulnerable. This reminds us that medical interventions are only part of the picture. Your underlying health, shaped by lifestyle medicine—nutrition, movement, sleep, stress—can be just as important as any pill or procedure.
Honesty and Humility: The Medical Professional’s Power
If you’re a healthcare provider, your greatest strength isn’t just your knowledge—it’s your honesty. Admitting uncertainty, learning from new data, and always asking, “Is this truly in the patient’s best interest?” are the hallmarks of ethical care. Research shows that the 2024–2025 COVID-19 vaccine, for example, offers about 33% effectiveness against emergency visits and up to 46% against hospitalization in older adults. These numbers matter, but so does the context: the patient’s age, immune status, and overall health.
Vaccine safety surveillance has become more transparent, with expanded public access to VAERS data and ongoing monitoring by the CDC and FDA. This shift towards openness is critical. It allows both patients and professionals to make decisions based on real-world evidence, not just assumptions or tradition.
Institutions: Reform and Patient-Centered Care
Healthcare institutions must move beyond one-size-fits-all solutions. Ongoing evidence review and broader reform are needed to curb preventable deaths and rebuild trust. That means prioritizing patient-centered care, where your unique needs and values are at the center of every decision. It also means being willing to change course as new research emerges—whether about vaccine safety, heart health, or any other aspect of public health.
Blending Innovation and Ancient Wisdom
The future of healthcare isn’t purely drug-based, nor is it entirely alternative. It’s a blend—a thoughtful mix of scientific advances, honest conversation, and old-fashioned prevention. Lifestyle medicine, which emphasizes daily habits and root-cause solutions, will play a larger role alongside new treatments and vaccines. Studies indicate that COVID-19 vaccination averted approximately 68,000 hospitalizations during the 2023–24 season, but prevention through healthier living remains just as vital.
Ultimately, your health is shaped by both the choices you make at home and the support you receive from the medical system. By staying proactive, skeptical, and empowered, you help create a future where public health is truly a partnership.
FAQ: Navigating Today’s Vaccine and Heart Health Landscape
If you’ve been following the headlines or talking with your doctor, you know that questions about COVID-19 vaccine safety, COVID-19 vaccine effectiveness, and the role of statins in heart health are more pressing than ever. In 2024, with new data, shifting expert opinions, and expanded access to vaccine safety monitoring tools like VAERS, you might feel overwhelmed by conflicting advice. Let’s break down the most common concerns and what the latest research—and real-world experience—can teach you.
Why are some doctors skeptical about new vaccines or statins? It’s not just about headlines or social media. Many doctors, including respected cardiologists like Dr. Aseem Malhotra, have voiced concerns due to past overpromises, unexpected side effects, and the strong influence of pharmaceutical marketing. Dr. Malhotra’s journey, shaped by personal loss and decades of clinical experience, highlights how systemic pressures can sometimes overshadow patient-centered care. When you hear skepticism, it often comes from a desire for more transparency and a return to medical ethics that put your well-being first.
How safe is the 2024–2025 COVID-19 vaccine? Research shows that the latest COVID-19 vaccines remain under rigorous safety monitoring. Both passive and active surveillance systems, including the expanded VAERS data access, report low rates of severe adverse effects. For example, the CDC and FDA have made it easier than ever for you to review vaccine safety data yourself. While some experts, like Dr. Malhotra, point to reanalyzed trial data suggesting higher-than-expected harm rates (1 in 800 for serious side effects), most public health agencies emphasize that these risks are rare compared to the benefits, especially for high-risk groups. Transparent data and ongoing Q&A remain crucial to public adaptation and trust.
What’s the single best way to avoid heart disease? Medication can help, but lifestyle is king. Regular physical activity, eating unprocessed foods, and reducing stress are the most powerful tools you have. Dr. Malhotra’s holistic approach aligns with robust evidence: 80% of heart disease risk is modifiable. Simple changes—like walking daily, cutting back on sugar and ultra-processed foods, and prioritizing sleep—can dramatically lower your risk. Don’t underestimate the impact of stress management, social connection, and even practices like meditation.
Are statins worth it? Statin facts can be confusing. For those with a history of heart attack or very high risk, statins may offer meaningful protection. But for most people without prior heart disease, the absolute benefit is small—sometimes as little as a few days of life extension over five years. Side effects, such as muscle pain and fatigue, are more common than many realize. It’s always worth having an open conversation with your doctor about your individual risks and alternatives.
Where can I compare vaccine side effect data myself? If you want to take charge of your health decisions, you now have more tools than ever. Public access to VAERS data, expanded in May 2025, allows you to review reports of vaccine side effects directly. This level of transparency is a major step forward for vaccine safety monitoring and helps restore trust by letting you see the data for yourself.
In the end, navigating today’s vaccine and heart health landscape means staying informed, asking questions, and weighing risks and benefits in the context of your own life. The call for transparency, humility, and open dialogue in medicine is not just about policy—it’s about empowering you to make the best choices for your health, now and in the future.
TL;DR: Beneath the heated headlines, today’s medical world faces a tug-of-war between pharmaceutical power, the evolving science of vaccines, and the timeless value of lifestyle. If you want real protection—for your heart, your future, and maybe even your peace of mind—it’s time to demand candor from the experts and your own habits.
Hats off to The Diary Of A CEO for the thought-provoking content! Take a look here: https://youtu.be/R87QLweXl1A?si=ay_MCNUsI6xifUnv.


Post a Comment